Leicester Medical School
Undergraduate simulation
- Simulation at the Midland Training and Simulation Centre, Queen's Hospital, Burton
- Simulation at Northampton General Hospital's simulation suite
 Inter-professional Teaching
Inter-professional Teaching
Inter-professional simulations bring the added advantage of combining the practice of university professional skills with team-working skills. In these simulations you will work and learn alongside students from other professions. These simulations have been found to be an excellent method for the development of non-technical or human-factor skills. These simulations also help to prepare you for practice within clinical settings.
Medical students are currently able to complete some of these simulations towards the end of their training and we are hoping to enable more opportunities throughout training.
 Junior Medicine Placement
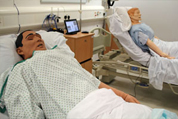
Junior Medicine Placement
Junior Medicine in the 3rd year of the course is one of the busiest blocks, as it aims to equip you with all the nuts and bolts of practising clinical medicine through working with one firm in an apprentice-style attachment.
In addition to consolidating how to take a history, examine patients and present your findings to senior colleagues, for many of you this will be first time you get to experience practical hands-on skills and develop management plans. Clinical simulation in the Junior Medicine block allows you the opportunity to put into practice many of the skills you learn during the block in a safe environment (for the patient and you) and we aim to cover many of the curriculum competencies.
The simulation programme aims to complement the on-the-job learning and experience that you gain, and all the skills you learn in the simulation lab can be taken back to your base wards, and are immediately relevant to good patient care.
 Junior Surgery Placement
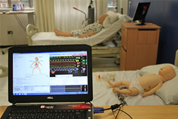
Junior Surgery Placement
Similarly, in 3rd year Junior Surgery you will have the opportunity to engage with scenarios that reinforce your experience of acute surgical admissions.
The management of surgical patients in the perioperative setting can be complex. Patients are often elderly, with multiple co-morbidities and are now undergoing increasingly major surgery. The patients may be 'nil-by-mouth', have IV fluids, catheters, NG tubes and drains. The perioperative surgical simulation sessions aim to complement what you see on the wards, and help your understanding of the management of common surgical scenarios using realistic cases that are seen day-to-day in the management of these patients on the wards.
 Specialty Placement Teaching - Child Health
Specialty Placement Teaching - Child Health
The first time you encounter a sick child can be a scary experience. The child health simulations provide an opportunity to manage sick children in a safe place so that you can feel more prepared when you enter the clinical environment. They also help you understand and develop some of the unique skill sets required for managing children and their families.
 Specialty Placement Teaching - Haematology
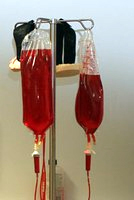
Specialty Placement Teaching - Haematology
Blood products are a valuable resource. UK red cells and other components are derived from a purely voluntary and shrinking donor population. Clinically inappropriate transfusion may cause harm to the patient and is a waste of a donation. Transfusion of incompatible products may lead to serious adverse reactions or death.
As a Foundation Doctor you will be ordering and prescribing blood products. You will also often be the first doctor called to assess a patient who is having a suspected adverse reaction to transfusion. Judicious use of blood products prolongs many patients' lives and transfusion can be immediately lifesaving in a situation of major blood loss or haemolysis.
This training package has been prepared and may be run by haematologists, transfusion practitioners and clinical skills facilitators. You will cover some common principles using clinical scenarios and gain practical experience of ordering and prescribing blood components and managing transfusion complications.
 Foundation Placements - Acute Care
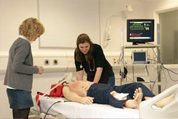
Foundation Placements - Acute Care
These simulations give you the chance to be on the medical front line. The simulations are set in the emergency department and provide you with the opportunity to manage medical emergency cases as they enter the front door. Like with any emergency department... who knows what problem you might encounter next?
 Preparation for Practice Simulations
Preparation for Practice Simulations
The simulation centre is converted into a 22-bed ward and you will be allocated to a team of junior doctors who will take handover and run the ward.
You need good diagnostic, practical, organisational, team-working and communication skills, with a good dollop of common sense, to see you through the maze of the clinical conundrum that you face. It is as close to real life as it can be. It is highly interactive.
This session gives you a chance to experience being an FY1 in the safety of the simulation centre. You have passed finals but are you ready for the challenge?
 Trauma Assessment and Resuscitation for Medical Students
Trauma Assessment and Resuscitation for Medical Students
We have designed a course to address trauma care called Trauma Assessment and Resuscitation for Medical Students (TARMS). This gives you some insight and understanding of the way that trauma care is delivered, and the opportunity to perform skills in a simulated environment.
The course is delivered by a multi-professional team of clinical skills facilitators from different backgrounds, and doctors from different specialties, including ED, pre-hospital care, trauma and orthopaedics.
Following an introductory lecture explaining the basics of trauma resuscitation, you are split into small groups and we cover different aspects of trauma care using simulated scenarios.
For example, you will cover separate aspects of traumatic injury assessment and resuscitation, and have the opportunity to practice simple life-saving skills. These include:
- Spinal immobilisation: collar fitting and log roll
- Chest: thoracocentesis and chest tube insertion
- Management of haemorrhage, including the insertion of interosseus needles