World’s first picture of the molecular machinery that makes cilia beat

Dr Robert Hirst
A picture of the structures that power human cilia – the tiny, hairlike projections that line our airways, has been produced by scientists for the first time.
The team of researchers, including Dr Robert Hirst from the University of Leicester, hope that the information could lead to much needed treatment for people with diseases of the cilia.
The study, published in Nature, combined advanced microscopy and artificial intelligence techniques to create a detailed snapshot of the structure of human cilia. These are the microscopic projections on the cells that line our lungs, ears and sinuses and beat rhythmically to keep the lungs clear from mucus and bacteria.
People who inherit the rare condition primary ciliary dyskinesia (PCD) have defective cilia that can’t effectively remove debris from the airways, and are at risk from repeated respiratory infections and pneumonia.
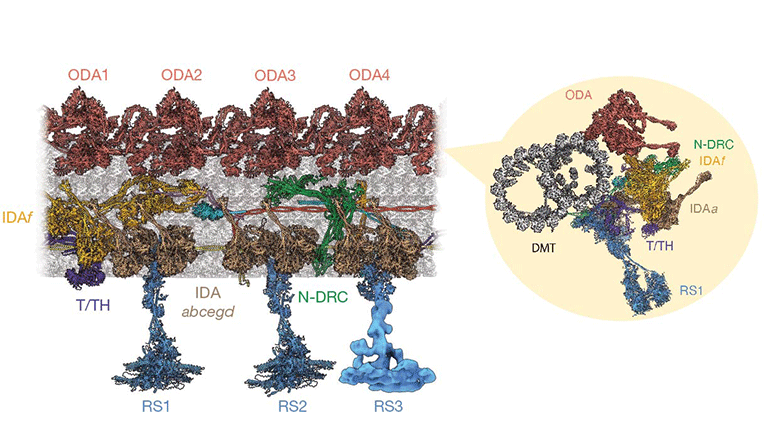
Now, for the first time, scientists have visualised the molecular ‘nano-machinery’ that causes cilia to beat, visible as identical structures dotted every 96 nanometres along the cilia length. These structures come together to form the axoneme. In healthy airways, this complex structure is tightly controlled, with molecules precisely arranged to make cilia beat in a rhythmic, wave-like motion, around a million times a day.
In people with PCD, the team found that cilia are unable to beat correctly because key elements of the axoneme structure are missing, caused by genetic mutations. This new information could lead to new medicines that target these defects, making cilia beat properly.Dr Robert Hirst, Principal Scientist at the Centre for PCD Diagnosis and Research, Department of Respiratory Sciences, at the University of Leicester who diagnosed and worked on the PCD cases is co-author on the paper.
He said: “The ability to understand how the molecular structure of motile cilia regulates cilia movement means we can apply this knowledge and the new techniques to increase our diagnostic power. This will help us, and others worldwide, to discover thousands of people living with PCD so we can provide them with appropriate therapy.”
Although relatively rare, affecting around 1 in every 10,000, the inherited disease is passed from parents to children through genes and is often difficult to diagnose, requiring complex tests.
Currently, there is no treatment to fix the cilia, but an early diagnosis enables patients to take precautions against infection and manage ways of keeping the airways and lungs as healthy as possible, preventing or delaying lung damage.
Researchers are still learning how the disease is inherited and which genes are involved.
Professor Hannah Mitchison from University College London’s (UCL) Great Ormond Street Institute of Child Health, co-authored the paper.
She said: “Treatments for PCD currently work to clear people’s airways and prevent infection. Our findings offer the possibility of molecular medicines to precisely target tiny defects in the axoneme and make cilia beat as they should.
“Molecular medicines are showing promise for other rare diseases, and COVID-19 research has unlocked new ways to deliver these drugs directly to the lung. If we can combine these advances with our new findings, my hope is that we’ll bring molecular medicines to people with PCD within the next five to 10 years.”
The team’s research could also prove useful for infertility, as sperm cells rely on a similar axoneme structure in their tails to propel themselves forward.
The research team was a global collaboration, with scientists based across the UK, US, Netherlands, China and Egypt.“It can be difficult to study rare diseases like PCD, because patients are spread thinly across the world. In the UK, we think around 9,000 families may be affected by PCD,” said Professor Mitchison.
“Our study was made possible by a fantastic international collaboration between clinical scientists, biologists and members of the rare disease community willing to take part in our research.”
The study involved collaborators at Harvard Medical School, Alexandria University, University of Leicester, Amsterdam University Medical Centers, Guy’s and St Thomas’ NHS Foundation Trust and Imperial College London.
At UCL, the study was supported by NIHR Great Ormond Street Hospital Biomedical Research Centre, the Ministry of Higher Education in Egypt and a MRC UCL Confidence in Concept grant.